TB Bug/Disease
Facts
 TB is a highly contagious infectious disease cause by the microorganism, Mycobacterium tuberculosis. According to the World Health Organization (WHO), worldwide TB kills more people annually than diarrhea + malaria + AIDS put together.
TB is a highly contagious infectious disease cause by the microorganism, Mycobacterium tuberculosis. According to the World Health Organization (WHO), worldwide TB kills more people annually than diarrhea + malaria + AIDS put together.
- High mortality (death) rate if untreated 1
- TB rate is falling but very slowly
- Large problem in prisons
WHO estimates a prison TB rate "100 times higher than that of the civilian population". Also, the TB incidence rate in prisons parallels that of human immunodeficiency virus (HIV) infection. The presence of these agents in the same person at the same time is referred to as a concurrent infection.
Other recent WHO statistics...
- ~ 1/3 world’s population is currently infected
- In 2008, estimated that 1.3 million people worldwide died from TB
- In 2009, ~10 million children worldwide became orphans as a result of TB
- In 2010, India & China accounted for 40% of world’s notified cases of TB
- In 2010, the TB mortality rate in China was 400X greater than in the United States
1 Morbidity (sickness) rate has an even greater effect upon local populations due to decreased work productivity.
Mycobacteria
Mycobacteria are unusual group of microorganisms sharing properties of both bacteria & fungi. There are only two significant human pathogens infecting normally healthy people:
- Mycobacterium tuberculosis (Koch’s bacillus- 1882 )
- Mycobacterium leprae (Hansen’s bacillus* - 1874)
* Causative agent of leprosy
Mycobacteria other than tuberculosis (MOTTS) are a group of environmental organisms associated with opportunistic infections in immunocompromised patients (e.g. AIDS). Mycobacteria marinum & Mycobacterium peregrinum are only two of several microbes making up this group. These organisms do not normally
infect healthy individuals.
TB Characteristics
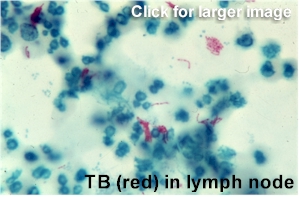
- Does not form spores (unlike anthrax)
- Often called acid fast bacillus (AFB) in medical settings
- Requires oxygen for its growth (obligate aerobe)
- Slow growing
- Resistant to drying & chemical disinfectants*
- Sensitive to heat (Pasteurization) & UV light
Disinfectants must list anti-mycobacterial, anti-tuberculocidal, or anti-TB (Tb) on their labels or they're no better at killing TB than is water, which doesn't hurt it. Also, a disinfectant must remain on the surface that's being treated for the specified amount of time stated on the label.
Transmission
TB spread occurs when a TB-infected person generates airborne droplets (droplet nuclei
or aerosols) when a coughing, sneezing, speaking or "spitting". These TB-containing
aerosols remain suspended in air indefinitely. TB infection occurs when an uninfected individual inhales droplet nuclei containing
the bacteria and becomes established in the body. The lungs are the primary infection
site but if left unchecked by the immune response the disease can spread to other
parts of the body.
Symptoms
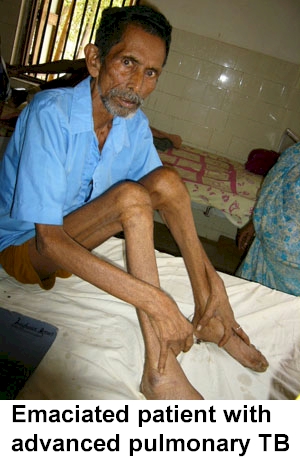
There are various symptoms that may indicate TB exposure. These may include:
- Lethargy (sluggish)
- Weakness
- Fatigue
- Fever
- Night sweats
- Weight loss*
- Persistent productive cough
- Coughing up blood or bloody-sputum (hemoptysis)
- Loss of appetite
* Consumption is the old name for tuberculosis (TB), which describes how the illness wastes away
or "consumes" its victims.
Disease
 The disease can exhibit several different stages. Disease progression depends largely
on amount of TB microbe exposure and current immune system function. Persons with
competent immune system response can sometimes kill the microbe or at least contain
it. The later response is referred to as a latent infection. During latency, the living TB organisms are held within small nodular, calcified
areas called tubercles, hence the name tuberculosis. The calcium content of these
nodules make them readily apparent on chest X-ray films to a competent radiologist
. Later on, the TB organisms can become "reactivated" when the immune system is sufficiently
weakened by another agent or disease. HIV and malignancies (cancers) are but two
of these reactivation culprits. Miliary TB is when the TB organisms have disseminated (spread) from the lung to other body areas
(e.g., liver, brain, skin, etc.) causing further disease.
The disease can exhibit several different stages. Disease progression depends largely
on amount of TB microbe exposure and current immune system function. Persons with
competent immune system response can sometimes kill the microbe or at least contain
it. The later response is referred to as a latent infection. During latency, the living TB organisms are held within small nodular, calcified
areas called tubercles, hence the name tuberculosis. The calcium content of these
nodules make them readily apparent on chest X-ray films to a competent radiologist
. Later on, the TB organisms can become "reactivated" when the immune system is sufficiently
weakened by another agent or disease. HIV and malignancies (cancers) are but two
of these reactivation culprits. Miliary TB is when the TB organisms have disseminated (spread) from the lung to other body areas
(e.g., liver, brain, skin, etc.) causing further disease.
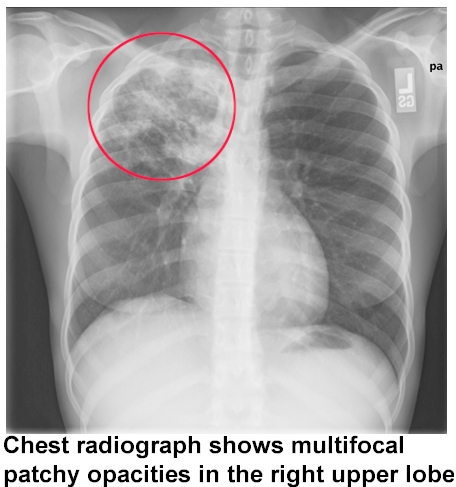
Image on right demonstrates multiple tubercles (opacities) in the red circled area.
Drug Resistant Strains3
TB bacteria is much more difficult to kill than most bacteria. Its elimination requires the use of multiple drugs for an extended period of time. Eventually, several TB strains have become resistant to several primary (first-line) medicines used to treat it. However, the primary reasons for TB microbes acquiring increased drug resistance are similar to those for increased bacterial antibiotic resistance. Antituberculosis medications are either misused or mismanaged, for example:
- Patients do not complete their full course of treatment
- Health-care providers prescribe wrong treatment...wrong dose... or wrong length of time for taking drugs
- Drug supply is not always available (large problem in developing countries)
- Poor quality drugs (unregulated manufacturing, storage, etc.)
A. Multidrug-Resistant TB (MDR TB)
Multidrug-resistant TB (MDR TB) have been noted for several years now. These are TB strains that demonstrate resistance "to at least two of the best anti-TB drugs, isoniazid and rifampicin. These drugs are considered first-line drugs and are used to treat all persons with TB disease". They are also less expensive than second-line drugs.
- Multidrug-Resistant TB (CDC Fact sheet)
B. Extensively Drug-resistant TB (XDR TB)
Extensively drug-resistant TB (XDR TB) is a relatively rare type of MDR TB. "XDR TB is defined as TB that is resistant to isoniazid and rifampin, plus resistant to any fluoroquinolone and at least one of three injectable second-line drugs (i.e., amikacin, kanamycin, or capreomycin)."
A large problem with XDR TB is their resistance to first-line and second-line drugs. This leaves patients with fewer treatment options all being much less effective.
- Extensively Drug-Resistant TB (CDC Fact sheet)
Go to next section: Training Requirements
